Wow, do I ever feel like I was thrown in at the deep end. The first two days of clinicals have been a great experience. I've had a chance to be exposed to many, MANY new things. I feel fortunate that my clinical group of eight students was assigned to a floor that has many clients with more complex care needs. I think many other groups have clients who are more able, but I was mainly with clients who need full care.

But it's been a little overwhelming. Today, I suctioned my first tracheostomy tube. I've seen more tracheostomies in the past two days than I ever wanted, plus some. I'd never even seen a tracheostomy before, much less cleansed, dressed and suctioned one. I never realized the vast quantities of colorful mucous that comes erupting, bubbling, spewing and projectile-launching out of them. It's not a pretty sight. Normally, our lungs make that much mucous, but we cough it up and swallow it, unaware. To suction a tracheostomy, you have to basically shove a vaccuum-cleaning suction catheter down the stoma (hole in the trachea) a LONG ways until the patient goes into violent gagging contorsions. Then using your thumb as a valve to apply suction, you slowly pull the catheter out. The entire procedure must be done with strict aseptic technique, sterile gloves and a sterile field. Mucous gets everywhere, so wear goggles or a full face mask.
Today, I watched as a wound care specialist dressed a decubitis ulcer (bedsore) that was so large and deep I could almost have put my fist in it. It was deeply undermined around the surrounding tissue. It was impressive that any pressure ulcer could get so large. It didn't bother me as much as the mucous from tracheosomies, though.
In the past two days, I've taken care of clients with tracheostomies, stomach tubes and urinary catheters. Some haven't been able to communicate at all, some have communicated vehemently that everything your are doing is wrong and some have been very pleasant and smiling. I shaved a guy for the first time (it is a very different experience!). I've dressed immobile clients, given bed baths, put on compression stockings and used hydrolic lifts to put clients in wheelchairs. I've emptied urine bags, brushed teeth, made beds, changed adult briefs (adult diapers) and combed hair. I assisted with a stretcher bath for a client today. We used a special stretcher lift to transport the client from the room to a spa tub in a bathing room. All of theses experiences were very hands-on. I was right there helping with the soaping and shampooing.
Communication has been a huge challenge. I've tried to understand the speach of clients with tracheostomies, and I've gotten better at lip reading. Some clients have really limited awareness. How do you communicate with them? How do you ask them permission to take a blood pressure or feel their pulses?
It's also brought to light some intense ethical considerations. How long do you maintain a client with no cognition on feeding tubes? At what point does quality of life deteriorate to a point where it shouldn't be maintained? If the individual still breaths independently, but needs supplemental oxygen, has no musculoskeletal movement, and has limited cognition, what then? The more I've seen, the more I know that I would never want to be maintained in this way. However, since they are not on ventilators, there is no easy switch to turn off.
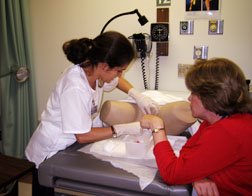
To add to a veneer of the surreal to the experience, it has all been done with Chuck Norris in the background. Many residents listen endlessly to daytime TV. All of these experiences have been done to Martha Stewart Living and various reruns of Days of Our Lives playing endless in the background. Here I am, looking official about 5 minutes after my second clinical.